Why welcoming my beautiful daughter into the world was the most terrifying day of my life
I almost died when my sweet baby girl was born at 27 weeks. It’s a miracle we both survived.
My friends and family have always said: “Lucy, you were born to be a mum.”
I wholeheartedly believe that to be true.
But it’s astonishing to me, to think that the very thing I was born to do almost killed me.
The most magical moment of my life was when I became a mum, in November 2019.
As I held my beautiful son in my arms, breathing in his gorgeous newborn scent, his tiny fingers wrapped tightly around mine, I felt a love like never before. In that moment, in my blissful baby bubble, I knew there was only one thing that could ever match that moment of magic: Giving Theo a brother or sister.
But that wasn’t something I expected to happen for a long, long time.
Towards the end of last year, I started to feel incredibly unwell. My first symptoms were intense stomach pains, quickly followed by excessive bleeding.
What I thought was a menstrual period seemed to roll into the next without a break. A couple of days would pass before my bleeding started again, just as persistently as before.
But it was only when I lost my appetite that I really began to worry. Upon researching my symptoms online, I quickly convinced myself I had a serious illness.
So, I booked a smear test, during which my practice nurse asked me if I could be pregnant. Given the fact that I was excessively bleeding and taking a daily contraceptive pill, I said no. She agreed it was unlikely.
It was an enormous relief when my smear results came back normal. Still, I was advised to do a pregnancy test, just to rule it out.
I was astonished when a positive result flashed at me, almost immediately. Still unconvinced, and without telling a soul, I booked a private scan.

“I don’t think you’ll see anything, I don’t actually think I’m pregnant,” I told the sonographer.
But the second the doppler hit my stomach, I could see a perfectly-formed baby on a big screen, right in front of me. My jaw dropped, and the tears flowed.
“This is a pretty advanced pregnancy, Lucy,” she replied, taking my baby’s measurements.
She confirmed I was approximately 20 weeks pregnant, with a healthy baby girl.
“Congratulations,” she said, replaying my little one’s heartbeat for me.
It was such a shock. How could I have not known? I’d known from day one with Theo.
But my baby girl was the sweetest, most wonderful surprise. I’d always dreamed of having a baby girl called Nina, so I felt as though my surprise pregnancy was simply meant to be.
I couldn’t wait to tell Theo he was going to be a big brother.
Later that night, I showed him my scan pictures. He danced around the room and gave my tummy a kiss.

The whole family was delighted, already counting down the days until she arrived.
Little did we know just how soon that would be.
Given that I had missed so many antenatal appointments and screenings, I was booked in for a scan at Whiston Hospital days later. Thankfully, despite my bleeding – and taking a contraceptive pill for the entire duration of my pregnancy – Nina was perfectly healthy.
I was however told that I had an extremely low-lying placenta, known as Placenta Praevia, and referred to a specialist consultant for further imaging.
I’d heard of Placenta Praevia before. I knew it was common in women who’d experienced a previous C-section, which I’d had with Theo, so I wasn’t worried – just so excited to have another peek at my baby.
By this time, my stomach had well and truly popped. Almost overnight, I looked as pregnant as I was.
It all seemed so surreal – the type of whirlwind story I was used to writing, but not living.
At my next scan I met my incredible consultant, Dr Agass, who specialises in placenta-related complications. As she started scanning, I knew something was wrong. The silence in the room was deafening.
She gently explained that she suspected I had a condition called Placenta Accreta, a serious pregnancy complication that occurs when the placenta grows too deeply into the wall of the uterus, sometimes attaching itself to nearby organs. Dr Agass explained I would need a planned C-section and, at the time of birth, I could require a full hysterectomy to save my life. I was at high risk of severe blood loss after delivery.
It quickly became apparent that the bleeding I’d experienced for months on end wasn’t down to periods or hormones, but a dangerous condition that could kill me. The very same pregnancy complication Kim Kardashian had, and the reason her subsequent two pregnancies were carried by a surrogate.
I felt like the walls were closing in on me, and a crushing fear overwhelmed me. I was petrified I’d die in childbirth, never meet Nina, never see Theo again.
I knew that my pregnancy could be my last, but I couldn’t quite enjoy it because I was so scared. Instead of counting down the days until I met my baby girl, I felt like I was counting down the days until my death.
Every night, I’d curl up beside Theo as he drifted off to sleep and cry, terrified I’d never live to see my beautiful, brilliant baby boy grow up.
Four weeks later, I was out with friends when I popped to the toilet. I was horrified to find I was bleeding.
I was rushed into hospital and kept in overnight for monitoring. Midwives and doctors believed it was old blood, given it was pretty dark, and nothing to worry about.
But exactly one week later, I started bleeding again and this time, the blood was fresh and red. I was once again rushed to hospital.
This time, I was given two steroid injections to help mature Nina’s lungs. It suddenly dawned on me that I could be having a very premature baby, and I was so frightened for her.
I used hashtags to find other parents of preemies on Instagram, and people who had been diagnosed with Placenta Accreta. The women I spoke to were incredible, a real pillar of support at such an uncertain time. However, it was terrifying to discover several had died in childbirth, and their accounts had been taken over by a partner or friend.
I spent two nights in hospital, before being discharged. Just hours after I got home, my bleeding resumed, so I spent another six hours in hospital. I was allowed home on the basis that I live two minutes away from the hospital.
“If your bleeding becomes even slightly heavier, you’re to come straight in,” my doctor said.
The following morning, I had the heaviest bleed I’d experienced to date. Dr Agass came to see me on the ward, and told me in no uncertain terms that I was staying in hospital until Nina arrived safely.
At just 26 weeks and four days pregnant, I had no idea how long I would be in hospital for. The thought of not seeing Theo for weeks after never spending more than one night apart broke my heart.
“What if I never see him again?” I fretted to my mum, as we video-called that night. I was absolutely petrified.
Two days later, I passed an enormous blood clot in the shower. This time, there was no sign of an end to my bleeding.
Within minutes, my room was full of midwives, doctors and registrars. They attempted to quantify my blood loss as they took my observations and hooked me up to the monitor to check on Nina.
“Little Nina is absolutely fine,” they assured me. “We will keep an eye on things overnight and reassess you in the morning.”
When a midwife came to check on me the next morning, I pushed myself up in bed. As a result of that small movement, I suffered a ‘mini haemorrhage’.
My room once again filled with specialists, who unanimously agreed to transfer me to the delivery suite.
“We don’t want to scare you and it doesn’t mean your baby is coming, but you’ll have one-to-one monitoring there,” they explained.
As I trembled with fear, my gorgeous midwives took it in turns to give me a cuddle and promised to look after me. I truly believed I was in the safest hands.
I bled all day, too scared to move in case I somehow made things worse. But I took great comfort in the knowledge that Nina was safe.
As the day wore on, I began to feel increasingly uncomfortable. My discomfort turned to severe pain, and I was convinced I had gone into labour. I was given gas and air, which was great for a while. But eventually, that too ceased to help.
I had a speculum examination, during which three large clots were removed. This temporarily eased my pain, but it was apparent things were taking a turn for the worst.
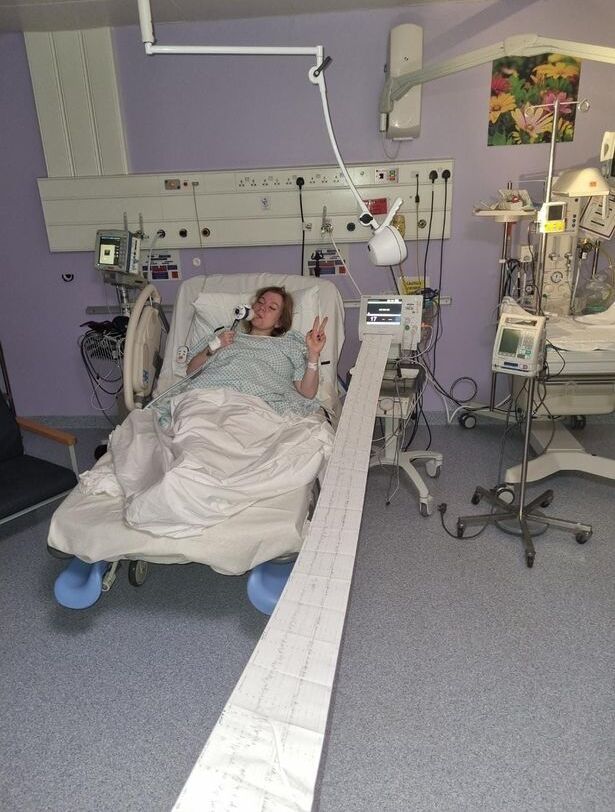
I was gowned up and put on the list for theatre after midwives calculated that throughout the course of the day, I had lost 800mls of blood. They explained that the safe amount of blood loss in childbirth is 1000mls – one litre – but I hadn’t given birth yet, and my blood loss was persisting.
I was given two magnesium sulphate injections to protect Nina’s brain from neurological damage, protect her intestines from a condition called NEC which can be fatal for premature babies, and give additional support to her tiny little lungs.
At this moment, I knew Nina was coming. I was terrified that it was far too early for her, terrified she wouldn’t survive, terrified that if she did, by some miracle, I wouldn’t – leaving my precious babies behind.
Before the second injection, I asked a midwife to roll me onto my side. I thought changing my position might help to ease my discomfort. But within seconds, I began to feel a bizarre sensation, almost as if my waters were breaking. Then, I felt something give.
Blood poured out of me like water from a tap, and the room was quickly filled with doctors, my anaesthetist, and a handful of neonatal nurses. Amidst the chaos, I heard a number of comments being passed around the room.
“We need to move, we need to get her to theatre now.”
“She’s losing too much blood, she’s going to collapse.”
“Look at the colour of her skin, we’re going to lose her.”
I glanced at my hands to find they had turned yellow. I later learned this was a symptom of haemorrhagic shock, a condition caused by severe blood loss. If not immediately treated, haemorrhagic shock is quickly followed by death.
I had my second injection, signed my consent forms for a C-section before I was rushed off to theatre, still completely lucid and aware of everything happening around me. The faces of the midwives we passed in the corridor confirmed my fears.
With one lovely midwife clutching my hand, I was lifted onto the operating table. I knew my consultant had been called in from home, but wasn’t yet present.
My anaesthetist, who ultimately saved my life, was the most gentle and calming presence.
“We’re advised to keep you awake, but my advice is that we put you to sleep for the procedure,” he told me softly.
I had complete trust in him, so I agreed. The last words I heard before I closed my eyes were: “There’s no heartbeat, you need to do something now.”
I remember thinking about Theo’s little face, and willing myself to survive for him and Nina. But I also prayed that if only one of us could survive, it would be her.
Then, I woke up in recovery, halfway through my fourth blood transfusion.
“Is Nina okay?” I murmured.
“She’s doing great,” a nurse replied, before I passed out again.
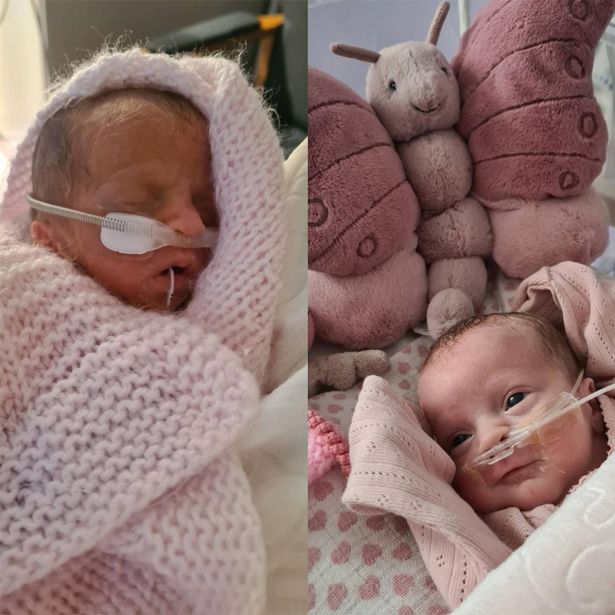
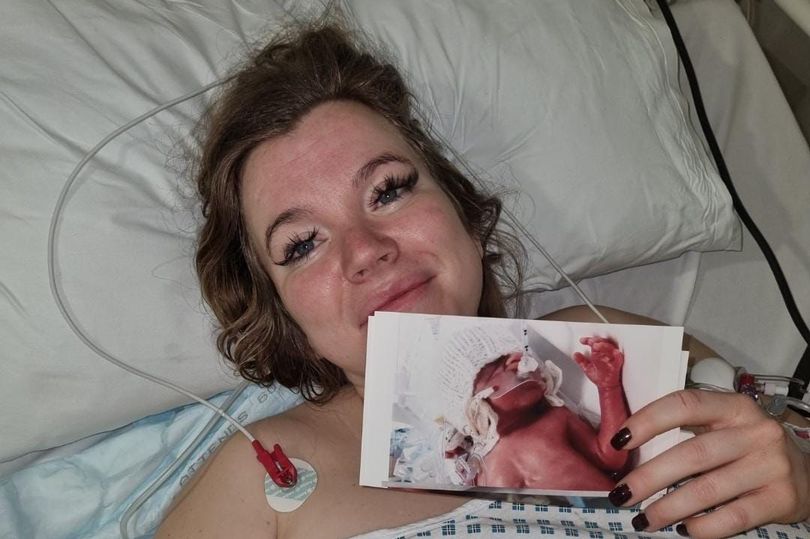
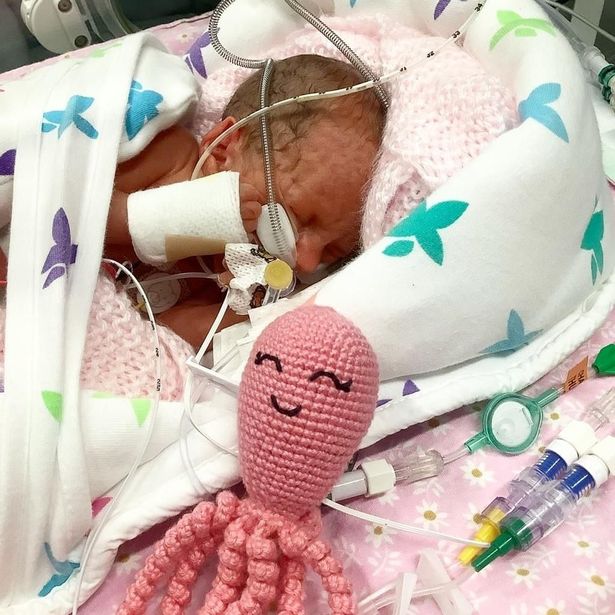
When I came around, she handed me a picture of Nina. Heartbreakingly small, surrounded by wires and intubated, yet perfect as could be.
It was later decided that she would be transferred to Liverpool Women’s Hospital, who were more experienced in handling babies born at such an early gestation.
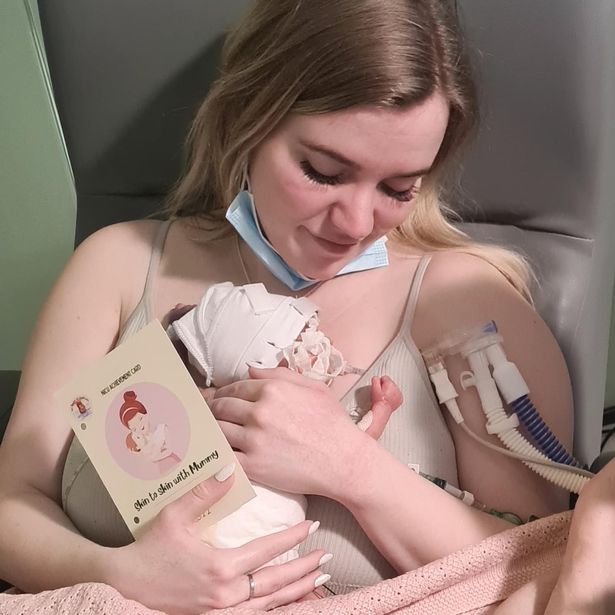
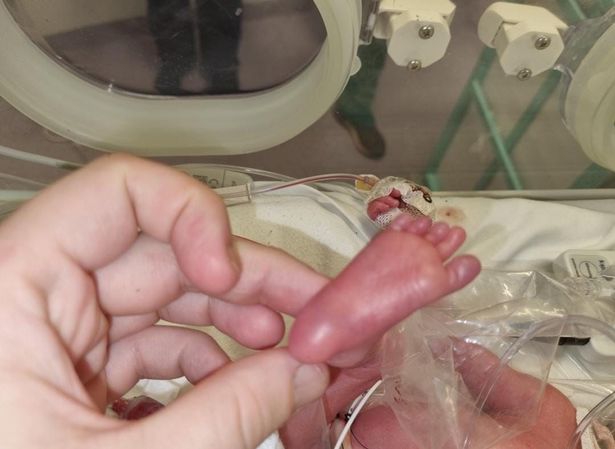
I was taken from the intensive care unit to meet her for the first time before her transfer. Weighing just 2lbs and 2oz, born at 27 weeks and one day, she weighed the same as a bag of sugar. Her little arms were no wider than her dad’s little finger.
“I love you so much, and I’m so proud of you, keep fighting,” I whispered through my tears.
In the hours that followed, I became increasingly unwell. Then, I was diagnosed with sepsis. I was devastated to learn Nina had sepsis too, as well as chronic lung disease and respiratory distress syndrome.
I received hourly updates via phone, whilst fighting to get my own strength back so that I could be with her.
I couldn’t breathe without oxygen, and my whole body shook violently. The pain across my fresh C-section wound was excruciating, and I had extreme post-traumatic stress disorder. Every time I felt I was bleeding, I was convinced I was going to haemorrhage again.
It broke my heart that I was so far from Nina, unable to cuddle and feed my baby, bonding like I should have been. So, I began to express breastmilk for her, which was transferred to her hospital and given to her via a feeding tube. Knowing that I was able to do something for Nina gave me the focus I needed – a welcome distraction from the reality of everything we’d both endured.
I had two more blood transfusions and various courses of antibiotics, and slowly started to feel better. The next day, one of my lovely midwives appeared in the doorway of my room.
“I’ve got a surprise for you,” she said.
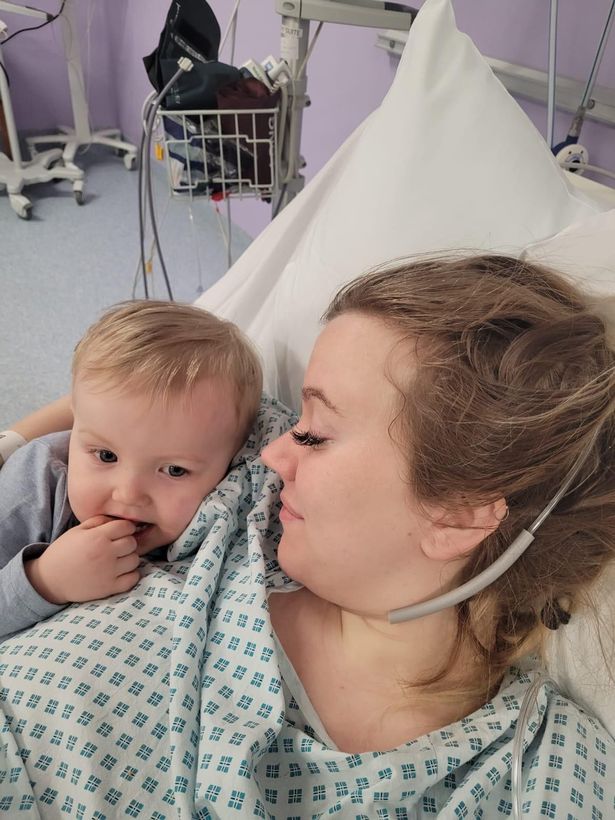
Then, I spotted Theo’s little boots under the curtain. I hadn’t seen him for a whole week, and it was exactly what I needed. He hadn’t been allowed to visit, but midwives made an exception because I was in my own room. They also believed the boost from spending time with him would speed up my recovery.
We had the most wonderful cuddle – something I had been certain would never happen again – and he was so happy to see pictures of his tiny baby sister. He couldn’t understand why she wasn’t with us, but I promised him he would meet her very soon.
“I love you, mummy,” he told me.
After two days at Liverpool Women’s Hospital, Nina returned to Whiston Hospital.
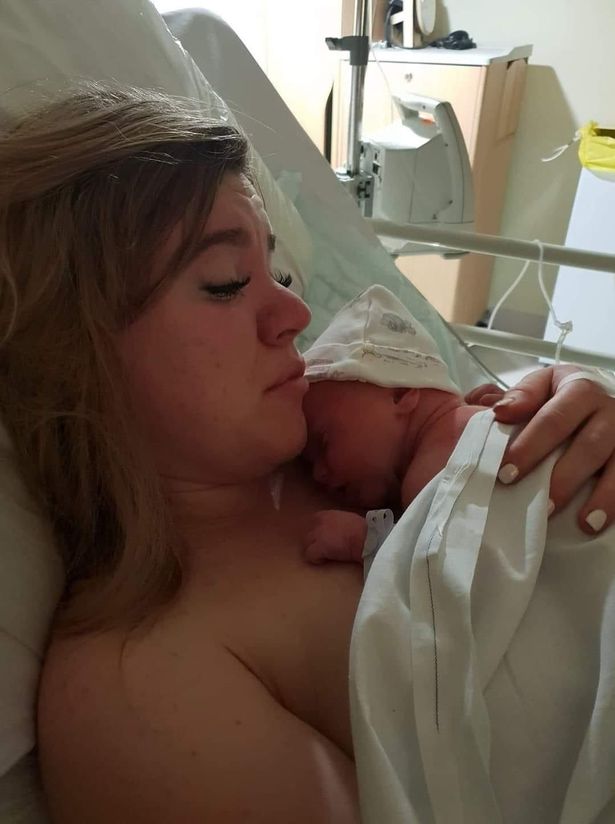
Nothing could ever describe the pain of seeing my baby’s tiny body covered in tubes and wires, machines doing for her what my body failed to. It was devastating in a way I had never experienced and it took my breath away, but I was so happy when a neonatal nurse asked if I wanted to hold her for the first time.
She was so tiny, I was terrified I’d break her. As she lay in my arms, like a little baby bird, I prayed she would be okay. After five days in hospital, I was discharged. The heartbreak of leaving the hospital without my baby is something I will never forget.
Two weeks later, Nina was diagnosed with a Patent Ductus Arteriosus (PDA), an extra blood vessel found in babies before birth and just after birth. In most babies who have an otherwise normal heart, the PDA will shrink and close on its own in the first few days of life. If it stays open longer, it may cause extra blood to flow to the lungs, resulting in them requiring respiratory support – a common occurrence in premature babies.
I was told it could be treated with ibuprofen or paracetamol and, failing that, a small surgical procedure to manually close it.
Nina was given ibuprofen, but it irritated her tummy, causing a bleed. This put Nina into distress, causing her to have several periods of apnoea. She was ventilated and transferred, once again, to Liverpool Women’s Hospital. I was devastated, but had total faith in my little fighter.
After a course of paracetamol, it was confirmed that the open valve had closed, and Nina was extubated. She was then transferred back to Whiston Hospital, where she began to thrive. First, she graduated from her incubator. Then, I was overjoyed to see her oxygen requirement decreasing by the day.
She was such an active and wriggly baby that she quickly earned herself the nickname ‘Nina Ballerina’. Every time I entered the neonatal unit, I could see her little legs performing acrobatics.
I was warned that it would be unlikely for Nina to come home before her due date, that she could require respiratory support for up to a year, and it would be almost impossible for me to breastfeed her – amongst countless other uncertainties.
Throughout her stay in the NICU, Nina had six blood transfusions, countless scans and tests, but was so brave and fought so hard.
After four weeks in the NICU, Nina started to hunt for milk when I placed her on my chest. After seven weeks, she came off her oxygen completely. Ten days later, she came home.
After weeks of suffering the inexplicable heartache of leaving my beautiful baby behind in the hospital, I finally got my magical moment. I had shown Theo pictures of Nina, and given him little fabric squares to cuddle so that she would recognise his scent, but he hadn’t been allowed to visit due to ongoing Covid-19 restrictions.
When he saw her for the first time, he could barely contain his joy. His little face was the purest expression of true love I have ever seen. He ran to her side, lay down with her, kissed her and said: “Hello Nina, I’m Theo, I love you.”
It was truly the happiest day of my life, and the most magical moment by far.
Nina is now six months old. She is still a little doll, weighing just 11lbs, but she is thriving. She has been discharged by all clinics, and we’re just about to embark on her weaning journey after I successfully established breastfeeding. She is the strongest person I know, and proof that miracles can, and do, happen.
I was recently invited back to the hospital, where I met with Dr Agass for a debrief on Nina’s birth. She explained that my uterus had become so irritated by all of the persistent bleeds that it had contracted, crushing the placenta. Despite the damage to my uterus, I didn’t require a hysterectomy after all.
In total, I lost 4.3 litres of blood. My circulating volume, at the time, was believed to be 5 litres. By the time I arrived in theatre, my heart rate had dropped to just 30 beats per minute and my blood pressure was virtually non-existent. I was so close to losing my life.
I was even more amazed to learn that my anaesthetist had told two junior doctors to start my surgery before my consultant had even arrived, a procedure she described to be “at the realms of their capability”.
They must have been so scared, but despite that, they saved our lives. I am so thankful to everyone at both Liverpool Women’s and Whiston Hospitals for everything they did for us. The midwives, doctors, neonatal nurses, my anaesthetist, consultants and even the cleaning staff who kept my spirits high when I was at my lowest moments.
They truly are superheroes. Without them, we wouldn’t be here today. I will never forget their kindness, and will hold each and every one of them in my forever thankful heart.
Lou x